What does a Authorization Coordinator do?
An Authorization Coordinator ensures that the proper processes are followed when granting access to systems, documents, or resources. This role often involves checking documents to verify that all required permissions are in place. They communicate with various departments to ensure that authorizations are granted according to company policies and legal requirements. This position is crucial in maintaining the security and efficiency of an organization.
The Authorization Coordinator works closely with team members from different departments. They often coordinate with IT, HR, and legal teams to facilitate the authorization process. This role also involves maintaining detailed records of all authorizations. They ensure that all documentation is accurate and up to date. This attention to detail helps prevent unauthorized access and ensures that all operations run smoothly. The Authorization Coordinator plays a key role in upholding the integrity of an organization’s security protocols.
How to become a Authorization Coordinator?
Becoming an Authorization Coordinator involves several steps that lead to a rewarding career. This role is key in healthcare, insurance, and other industries where handling authorizations is crucial. Here are the steps to help anyone interested in this path take the right actions.
First, gaining the necessary education is important. Most employers require a high school diploma or equivalent. Some positions may also ask for a postsecondary certificate or an associate degree in a related field. Taking courses in medical terminology or office administration can be beneficial.
- Get an Education: Start with a high school diploma. Consider further education like a certificate or associate degree.
- Learn Medical Terms: Take courses in medical terminology to understand common terms.
- Gain Experience: Look for jobs or internships in healthcare or insurance to build your skills.
- Develop Skills: Improve skills in communication, attention to detail, and computer proficiency.
- Apply for Jobs: Use job boards and company websites to find openings. Tailor your resume to highlight relevant experience and skills.
How long does it take to become a Authorization Coordinator?
The journey to becoming an Authorization Coordinator can vary based on several factors. Typically, this role requires a high school diploma or equivalent as the basic educational requirement. From here, job seekers may pursue additional training or education to improve their qualifications. Some positions may prefer or require a college degree in a related field such as health care administration or business.
Most Authorization Coordinators gain experience through on-the-job training or internships. This hands-on experience helps them learn the specific tasks and responsibilities of the job. Experience levels can range from a few months to a couple of years. Certain employers may offer certification programs to enhance skills and knowledge. Completing these programs can make candidates more competitive in the job market. The exact timeline can differ depending on the individual's educational path and work experience.
Authorization Coordinator Job Description Sample
The Authorization Coordinator is responsible for managing the authorization process for clients or patients, ensuring that all necessary documentation and approvals are obtained and processed efficiently. This role involves collaborating with various departments and stakeholders to facilitate the authorization of services, treatments, or procedures.
Responsibilities:
- Verify and process client/patient authorizations for services, treatments, or procedures.
- Communicate with healthcare providers, insurance companies, and other relevant parties to obtain necessary documentation and approvals.
- Maintain accurate and up-to-date records of authorization statuses and related documentation.
- Identify and resolve any issues or delays in the authorization process promptly.
- Collaborate with billing and claims departments to ensure that all services are appropriately authorized before delivery.
Qualifications
- High school diploma or equivalent required; associate’s or bachelor’s degree in a related field preferred.
- Minimum of 2 years of experience in a healthcare or related authorization role.
- Strong knowledge of healthcare regulations, insurance policies, and authorization processes.
- Excellent communication and interpersonal skills to effectively interact with clients, providers, and insurance companies.
- Proficient in using computer applications, including Microsoft Office and electronic health record (EHR) systems.
Is becoming a Authorization Coordinator a good career path?
An Authorization Coordinator plays a key role in many organizations. They ensure that all necessary permissions and approvals are in place for various processes. This job involves working closely with different departments to streamline operations. It requires a strong attention to detail and good organizational skills.
There are several benefits to working as an Authorization Coordinator. This role offers stability and the chance to work with a variety of tasks. Coordinators often enjoy a diverse work environment. They interact with different teams and learn a lot about the company's operations. However, there are also some challenges to consider. The job can be repetitive at times, and managing multiple tasks can be stressful. Understanding these pros and cons helps job seekers make informed decisions about this career path.
When thinking about the pros of being an Authorization Coordinator, one should note:
- Stability: This role often offers job security.
- Variety: The job involves many different tasks and interactions.
- Learning Opportunities: Coordinators gain knowledge about various departments.
On the other hand, here are some cons:
- Repetitiveness: The job can feel monotonous.
- Stress: Handling multiple tasks can be challenging.
- Interpersonal Dynamics: Working with different teams can sometimes be tough.
What is the job outlook for a Authorization Coordinator?
The job outlook for Authorization Coordinators shows a steady demand within the industry. The Bureau of Labor Statistics (BLS) reports an average of 600 job positions opening each year. This indicates a reliable number of opportunities for those seeking to enter this field. However, it's important to note a projected decrease of 5.9% in job openings from 2022 to 2032, as reported by the BLS. This change suggests a need for job seekers to stay informed and adaptable in their career paths.
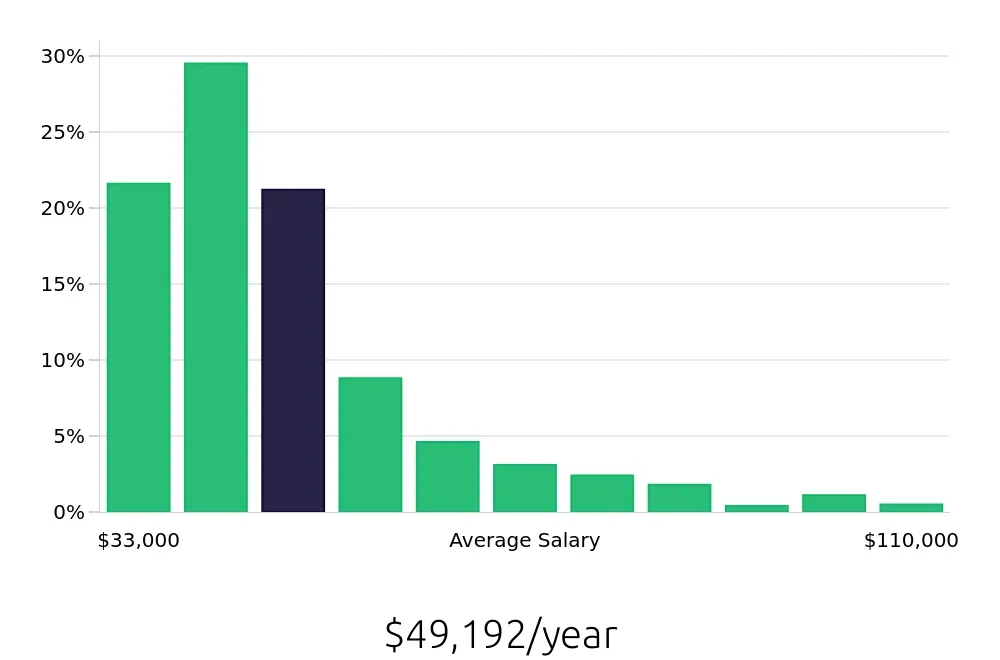
For those considering this role, the compensation is competitive. The BLS reports an average national annual salary of $46,940. This figure provides a clear picture of the earnings potential in this profession. Additionally, the average hourly wage stands at $22.57, reflecting the value placed on the skills and responsibilities of Authorization Coordinators. These figures highlight a rewarding financial aspect of the job, making it an attractive option for many job seekers.
In summary, while the job outlook for Authorization Coordinators shows some decline, the role remains a viable career choice. With an average of 600 positions opening annually and competitive compensation, this field offers stability and growth potential. Job seekers should focus on developing relevant skills and staying updated on industry trends to navigate this evolving job market effectively.
Currently 148 Authorization Coordinator job openings, nationwide.
Continue to Salaries for Authorization Coordinator