What does a Claims Examiner do?
A Claims Examiner plays a key role in the insurance industry. They review claims from policyholders to determine the validity of their requests. The examiner analyzes documents and gathers information to make informed decisions. Effective communication is essential as they may need to interact with policyholders, adjusters, and other team members. This position demands a strong attention to detail and the ability to make fair and accurate assessments.
The Claims Examiner examines the circumstances surrounding each claim. They assess the extent of the damage or loss and compare it with the policy details. This process involves careful investigation and fact-finding. The examiner must verify information and ensure all criteria are met. Accuracy and efficiency are crucial to avoid delays and maintain customer satisfaction. A Claims Examiner works to resolve claims promptly and fairly, contributing to the smooth operation of the insurance process.
How to become a Claims Examiner?
Becoming a Claims Examiner is a rewarding career choice for those interested in insurance and problem-solving. This role involves evaluating insurance claims to decide on the settlement amount. To embark on this career path, follow these steps:
- Earn a High School Diploma or GED: Begin with a solid educational foundation. A high school diploma or GED is the first step.
- Pursue Relevant Education: Consider a college degree in business, finance, or insurance. Some employers may require an associate or bachelor's degree.
- Gain Work Experience: Work in customer service or a related field. Experience in handling customer inquiries and resolving issues can be beneficial.
- Obtain Certification: Get certified through organizations like the American Institute for Chartered Property Casualty Underwriters (CPCU). This certification can enhance job prospects.
- Apply for a Position: Look for job openings as a Claims Examiner. Submit a resume and cover letter that highlight relevant experience and skills.
Following these steps can help job seekers successfully become a Claims Examiner. This career offers opportunities for growth and the chance to help people during challenging times.
How long does it take to become a Claims Examiner?
Pursuing a career as a Claims Examiner can lead to a rewarding role in the insurance industry. Many find it satisfying to help others during tough times. The journey to this career, however, requires some dedication and planning. Most people start by getting a high school diploma or GED.
After that, gaining the right experience and education is key. Some people choose to earn an associate's or bachelor's degree in business or a related field. This can take two to four years. Others may take courses in insurance or claim processing. This can help them understand the basics of the job. Most employers prefer candidates with some college education or specialized training. This can include a certification in insurance or claim processing.
Claims Examiner Job Description Sample
As a Claims Examiner, you will be responsible for evaluating, processing, and documenting insurance claims. You will ensure that claims are processed accurately and efficiently, and you will communicate with policyholders to resolve any issues related to their claims. This role requires attention to detail, strong analytical skills, and the ability to work under pressure.
Responsibilities:
- Evaluate insurance claims to determine coverage and liability based on policy terms.
- Review and analyze claim documents, reports, and other relevant information to make informed decisions.
- Communicate with policyholders, witnesses, and other parties involved in the claims process.
- Investigate claims to identify fraud or suspicious activities and report findings to the appropriate department.
- Prepare and issue settlement offers to claimants based on the analysis of claims.
Qualifications
- Bachelor’s degree in Business Administration, Finance, or a related field is preferred.
- Minimum of 2-3 years of experience in claims examination or a similar role.
- Strong understanding of insurance policies, terms, and conditions.
- Excellent analytical and problem-solving skills.
- Proficient in Microsoft Office Suite and claims management software.
Is becoming a Claims Examiner a good career path?
A Claims Examiner plays a crucial role in the insurance industry. They assess insurance claims to decide whether to approve or deny them. This role involves analyzing documents, interviewing policyholders, and consulting with adjusters. The goal is to ensure accurate and fair compensation for legitimate claims. Working as a Claims Examiner offers several benefits and a few challenges to consider.
One major advantage of this career is job stability. Insurance is a consistent industry, offering a steady demand for Claims Examiners. This role provides opportunities to work in various sectors, including health, property, and auto insurance. Additionally, Claims Examiners can advance in their careers by moving into management or specialized roles. This career path also allows for developing strong analytical and decision-making skills. However, it is important to consider some challenges as well. The job can be stressful due to the need for quick and accurate decisions. Long hours and tight deadlines are common. Additionally, some claims may be complicated, requiring extensive research and attention to detail.
Here are some pros and cons to consider:
- Pros:
- Job stability
- Opportunities for advancement
- Skill development
- Cons:
- Stressful work environment
- Long hours and tight deadlines
- Complex and demanding cases
What is the job outlook for a Claims Examiner?
The role of a Claims Examiner continues to be a stable and vital part of the insurance and financial sectors. According to the Bureau of Labor Statistics (BLS), approximately 21,500 job positions open up each year. This steady demand reflects the ongoing need for professionals who can accurately assess insurance claims and ensure fair settlements.
Despite a projected percent change of -3.1% in job openings from 2022 to 2032, the role remains essential. This slight decrease does not diminish the importance of Claims Examiners. Instead, it suggests a more streamlined approach to claims processing, emphasizing efficiency and technological integration. Job seekers can find comfort in the consistency and reliability of this career path, even as the industry evolves.
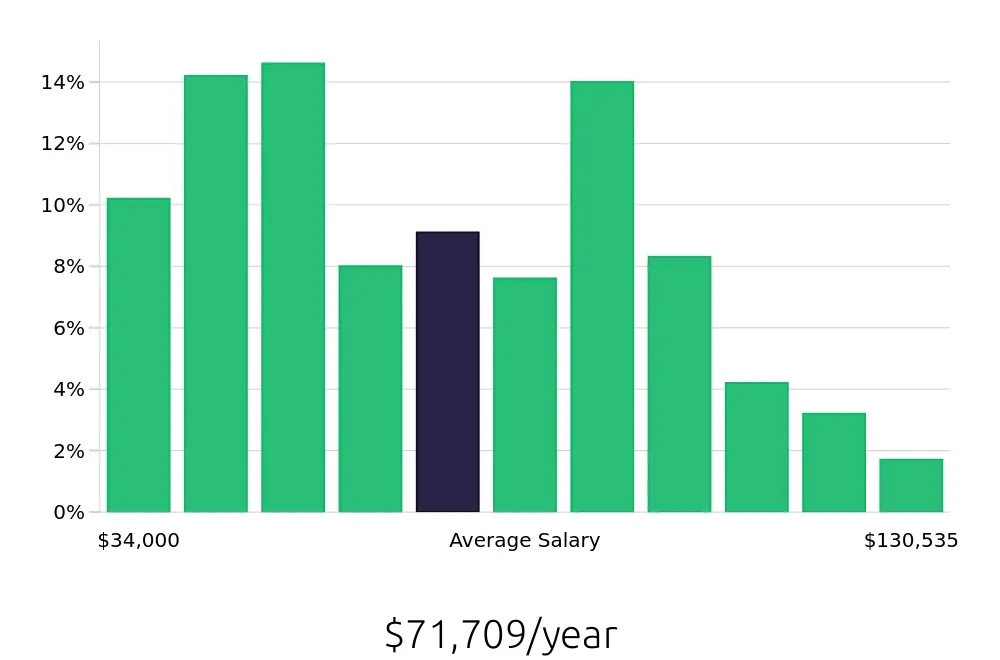
Claims Examiners enjoy a strong compensation package as well. The average national annual salary stands at $75,760, and hourly rates are approximately $36.43. These figures highlight the value placed on this profession by employers. For those looking to enter or advance in this field, the financial rewards are both attainable and rewarding. The BLS provides detailed insights into these figures, making it a valuable resource for anyone considering this career.
Currently 208 Claims Examiner job openings, nationwide.
Continue to Salaries for Claims Examiner