What does a Claims Processor do?
A Claims Processor plays a key role in managing insurance claims. This professional reviews claims submitted by policyholders. They verify the details of each claim. Next, they decide whether the claim is valid. They calculate the amount to be paid. The Claims Processor then processes payments to the policyholders. Accuracy and attention to detail are crucial in this job.
The Claims Processor also communicates with policyholders. They provide updates on the status of their claims. They answer any questions the policyholders might have. Clear and professional communication helps to maintain good relationships with clients. The Claims Processor uses various software tools to manage claims efficiently. They ensure that all claims are processed promptly. This role is essential in helping policyholders get the compensation they need.
How to become a Claims Processor?
Becoming a Claims Processor is a rewarding career path. It involves reviewing and handling insurance claims. This job is crucial in the insurance industry. Many people depend on Claims Processors to get the help they need.
Here are the steps to start this career:
- Earn a High School Diploma. The first step is to complete high school. A diploma opens the door to further education or training.
- Get Relevant Education or Training. Consider taking courses in business, insurance, or a related field. This can be through community colleges or vocational schools.
- Gain Experience. Look for jobs in administrative roles. Experience in customer service or data entry is valuable.
- Get Certification. While not always required, certification can boost your resume. The Claims Adjustment Specialist (CAS) credential is a good option.
- Apply for a Job. Start applying for Claims Processor positions. Use your education, experience, and certification to your advantage.
How long does it take to become a Claims Processor?
Getting a job as a Claims Processor can be a smart choice. Many people find this role both rewarding and manageable. The time it takes to become one can vary. Usually, it takes about one to two years. This includes any necessary education and training. Some steps might take less time while others could take longer.
First, a high school diploma is needed. Most employers require this basic level of education. Some jobs might ask for a GED if a diploma isn’t available. Next, job seekers often take additional courses. These could be at a community college or an online school. These courses cover topics like insurance and computer skills. They can also provide certifications. Some roles might need a bachelor's degree in a related field. This can take two to four years. However, many Claims Processors start their career with just a high school diploma and some training.
Claims Processor Job Description Sample
We are seeking a detail-oriented and efficient Claims Processor to join our team. The successful candidate will be responsible for evaluating and processing insurance claims with accuracy and timeliness. This role involves interacting with clients, verifying claims information, and coordinating with various departments to ensure that claims are settled promptly and fairly.
Responsibilities:
- Evaluate and process insurance claims by reviewing and analyzing claim documents, policies, and related information.
- Communicate with claimants to obtain additional information, if necessary, and provide updates on the status of their claims.
- Verify the accuracy and completeness of claims information and ensure compliance with company policies and regulations.
- Coordinate with internal departments, such as underwriting, risk management, and legal, to determine the validity and settlement of claims.
- Prepare and issue payment to claimants in accordance with policy terms and conditions.
Qualifications
- High school diploma or equivalent; bachelor’s degree in business, insurance, or a related field is preferred.
- Previous experience in claims processing or a similar role within the insurance industry.
- Strong understanding of insurance policies, procedures, and terminology.
- Proficient in using claims processing software and Microsoft Office Suite.
- Excellent analytical, problem-solving, and decision-making skills.
Is becoming a Claims Processor a good career path?
A career as a Claims Processor involves reviewing and evaluating insurance claims to determine their validity. This role plays a crucial part in the insurance industry, ensuring that policyholders receive the compensation they are entitled to. Claims Processors interact with clients, gather necessary documentation, and communicate decisions. This role is vital for maintaining the smooth operation of insurance companies.
Interested parties often find this career rewarding due to its direct impact on helping others and its stable demand. The job typically requires strong analytical skills and a solid understanding of insurance policies. Most employers prefer candidates with a high school diploma and relevant experience. Some positions may demand additional certifications or degrees.
Here are some pros and cons to consider before pursuing this career:
- Pros:
- Stability: The insurance industry is stable, offering job security.
- Helping Others: This role directly assists individuals in times of need.
- Clear Career Path: Experience can lead to promotions to managerial roles.
- Cons:
- Stressful: Handling claims can be high-pressure, especially with tight deadlines.
- Detail-Oriented: This job demands great attention to detail to avoid errors.
- Limited Advancement: Opportunities for promotion can be competitive.
What is the job outlook for a Claims Processor?
Job seekers looking to enter the insurance industry may find a promising career as a Claims Processor. This role involves handling and processing insurance claims. The Bureau of Labor Statistics (BLS) reports that there are about 22,100 job positions available each year for Claims Processors. Although the job openings are expected to decrease by 3.2% from 2022 to 2032, the demand for qualified professionals remains steady. This makes it a stable career path for those with the right skills and experience.
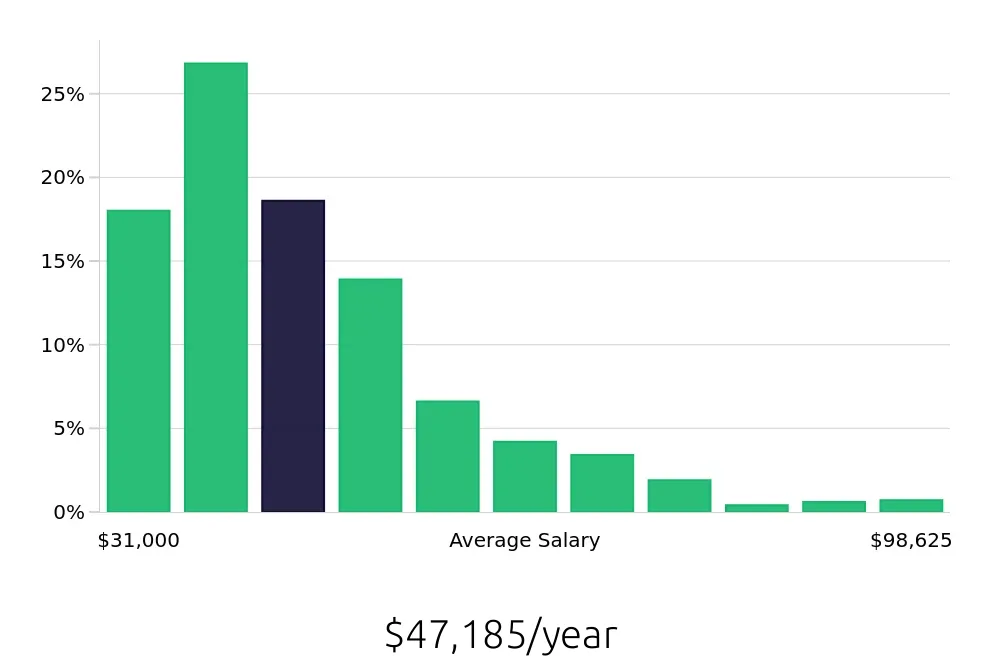
Applicants can expect a competitive salary for this role, with the average national annual compensation being $49,530. Hourly compensation averages around $23.81. These figures reflect the importance of Claims Processors in ensuring smooth operations within insurance companies. They also highlight the potential for growth and stability within the industry. A steady salary and the chance to advance in a dynamic field make this career attractive to job seekers.
The role of a Claims Processor offers a blend of opportunities for career growth and stability. Candidates who enter this field can look forward to a fulfilling career with the potential for advancement. Whether you are a new graduate or a seasoned professional, the skills gained in this role can open doors to higher positions within the industry. The insurance sector’s reliance on competent Claims Processors ensures job security and growth potential in this role.
Currently 206 Claims Processor job openings, nationwide.
Continue to Salaries for Claims Processor