What does a Clinical Appeals Reviewer do?
A Clinical Appeals Reviewer plays a crucial role in ensuring fairness in healthcare decisions. This professional reviews and evaluates appeals related to healthcare services and coverage. They assess the medical necessity of treatments and ensure that clinical decisions align with established guidelines and policies. By carefully analyzing medical records and other relevant data, the reviewer makes recommendations that support or deny appeals based on clinical merits.
Responsibilities of a Clinical Appeals Reviewer include conducting thorough reviews of patient cases, consulting with medical experts, and maintaining a strong understanding of healthcare regulations. The reviewer ensures that each appeal is handled with a high level of accuracy and attention to detail. Their work helps patients receive the appropriate care and ensures that healthcare providers adhere to best practices. This role requires strong analytical skills, a deep understanding of clinical guidelines, and the ability to communicate effectively with healthcare professionals.
How to become a Clinical Appeals Reviewer?
Becoming a Clinical Appeals Reviewer is a rewarding career path for those passionate about healthcare and detail-oriented work. This role involves reviewing and evaluating appeals from patients or providers regarding denied claims.
To start this journey, one needs to follow several steps that ensure a solid foundation in the necessary skills and qualifications.
- Obtain a relevant degree: Start with a degree in healthcare or a related field. This provides a basic understanding of medical terminology and practices.
- Gain experience: Work in a healthcare setting to understand patient care and claim processing. Experience in medical coding or billing is also helpful.
- Learn about healthcare regulations: Familiarize yourself with healthcare laws and regulations. Knowledge of coding guidelines and reimbursement processes is crucial.
- Pursue certification: Consider getting certified as a Professional Appeal Representative (PAR) or a similar credential. This adds credibility to your resume.
- Apply for positions: Look for job openings at hospitals, insurance companies, or medical review firms. Tailor your resume to highlight relevant skills and experiences.
How long does it take to become a Clinical Appeals Reviewer?
Interest in becoming a Clinical Appeals Reviewer has grown over the years. The journey into this profession can vary in length. Most find that the timeline stretches between one to three years. This period includes both formal education and hands-on experience.
To start, one may need a bachelor’s degree in a health-related field. Programs often include courses in medical terminology, healthcare systems, and patient care. Some employers may prefer or require additional certification in health information management. Clinical Appeals Reviewers must also gain experience. They may work in entry-level roles within healthcare or insurance. Gaining a strong understanding of clinical procedures and healthcare policies takes time. This hands-on experience is key to mastering the job duties.
Clinical Appeals Reviewer Job Description Sample
The Clinical Appeals Reviewer is responsible for evaluating clinical appeals related to healthcare services, insurance claims, and medical necessity. This role requires a deep understanding of clinical practices, healthcare policies, and insurance regulations to ensure fair and accurate review of appeals.
Responsibilities:
- Review and assess clinical appeals to determine the validity of the claims.
- Collaborate with medical professionals and insurance providers to gather necessary clinical information.
- Analyze medical records, treatment plans, and other relevant documentation to support appeal decisions.
- Communicate findings and recommendations to the appeals committee and stakeholders.
- Ensure compliance with healthcare policies, insurance guidelines, and regulatory requirements.
Qualifications
- Bachelor's degree in Healthcare Administration, Nursing, or a related field.
- Certification in a relevant area (e.g., CRC, ACM, CPHQ) is highly preferred.
- Minimum of 3 years of experience in a clinical or healthcare review role.
- Strong understanding of healthcare policies, insurance regulations, and clinical practices.
- Excellent analytical and critical thinking skills.
Is becoming a Clinical Appeals Reviewer a good career path?
A Clinical Appeals Reviewer examines cases where patients or providers have questioned the decisions made by healthcare insurers. This role involves reviewing medical records, understanding clinical decisions, and working to ensure that the outcomes are fair and justified. This position often requires a background in healthcare, such as nursing or medical coding, combined with an understanding of insurance policies.
Working as a Clinical Appeals Reviewer can be both rewarding and challenging. This role provides an opportunity to directly impact patient care and insurance outcomes. The job allows one to use medical knowledge in a different context, often leading to a deeper understanding of the healthcare system. However, it can also be demanding, requiring attention to detail and the ability to work under pressure.
Here are some pros and cons to consider:
- Pros:
- Opportunity to improve patient care by ensuring fair insurance decisions.
- Uses healthcare knowledge in a unique and impactful way.
- Potential for professional growth and specialization.
- Cons:
- Can be stressful due to the need for detailed analysis and quick turnaround times.
- Requires a deep understanding of both clinical practices and insurance policies.
- May involve working with sensitive and confidential information.
What is the job outlook for a Clinical Appeals Reviewer?
The job outlook for Clinical Appeals Reviewers is promising, with about 2,100 positions expected annually. This consistent demand indicates a stable career path for professionals entering this field. A forecasted job openings percent change of 2.4% from 2022 to 2032 adds to the positive outlook. This growth suggests an increasing need for skilled reviewers in healthcare settings.
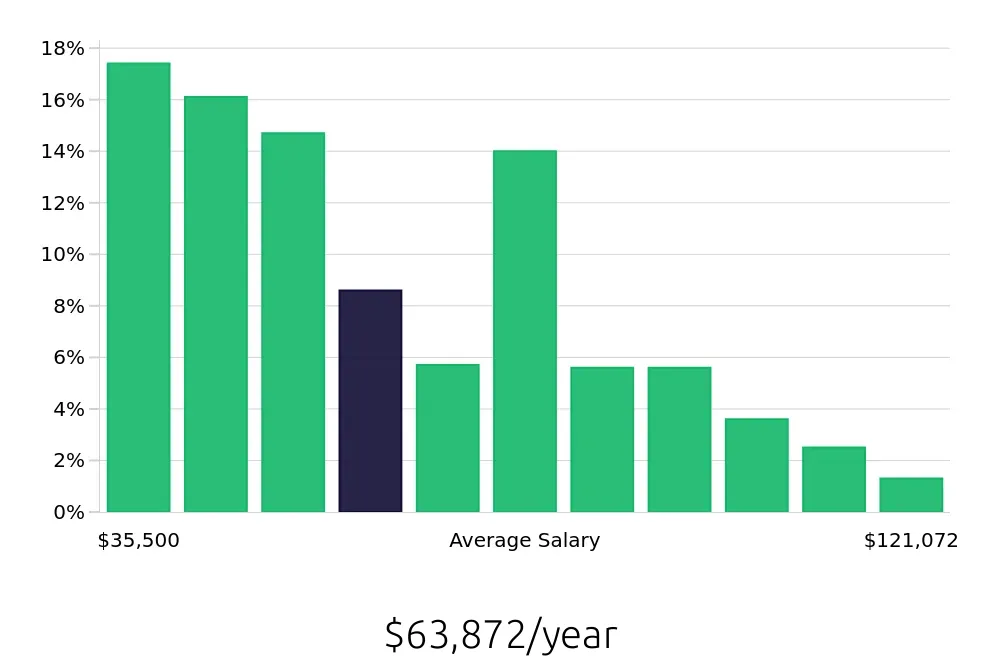
Clinical Appeals Reviewers enjoy a strong compensation package. The average national annual salary stands at $126,270, reflecting the value placed on these roles. Additionally, the average national hourly wage is $60.71, providing financial security and stability. These figures make a career as a Clinical Appeals Reviewer both attractive and rewarding.
Overall, the field of Clinical Appeals Reviewing offers a blend of job stability, good compensation, and positive growth. Job seekers with the right skills and certifications can look forward to a fulfilling and lucrative career in this profession. The combination of steady job availability and strong earnings potential makes this a smart career choice.
Currently 77 Clinical Appeals Reviewer job openings, nationwide.
Continue to Salaries for Clinical Appeals Reviewer