How much does a Clinical Appeals Reviewer make?
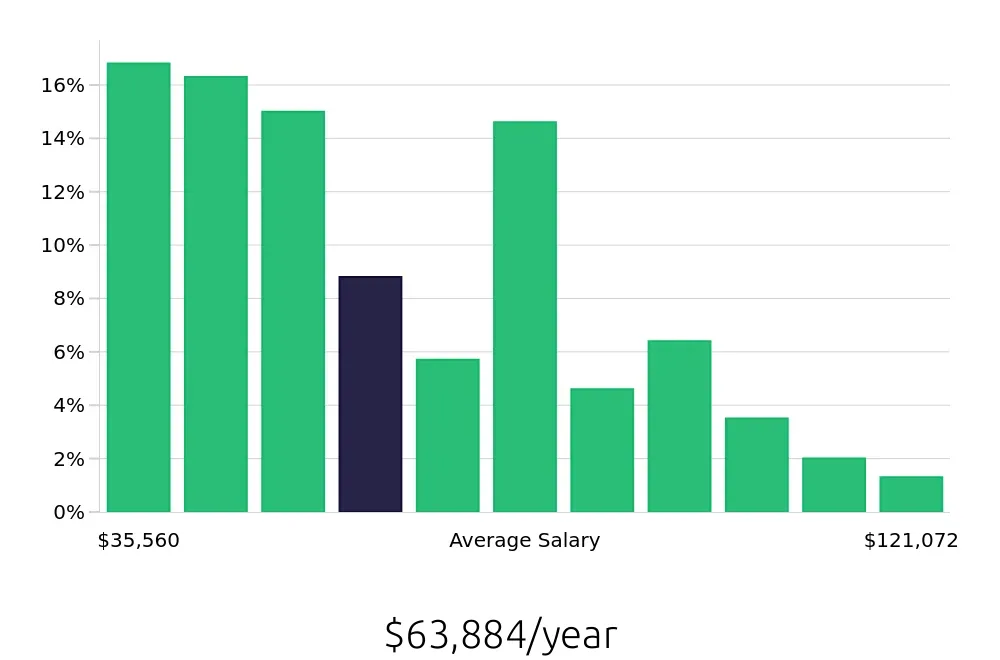
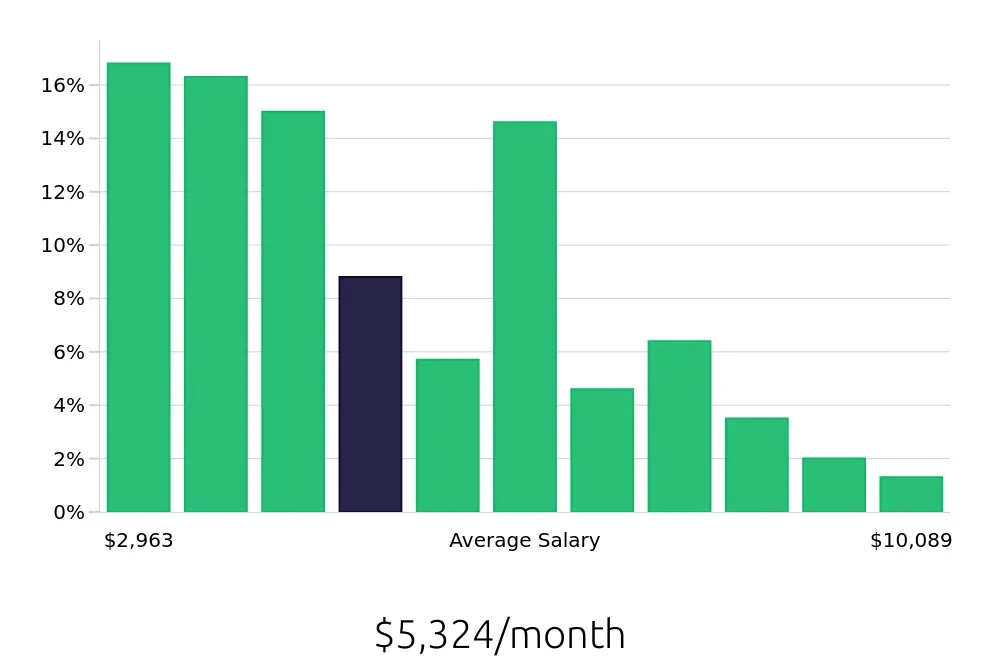
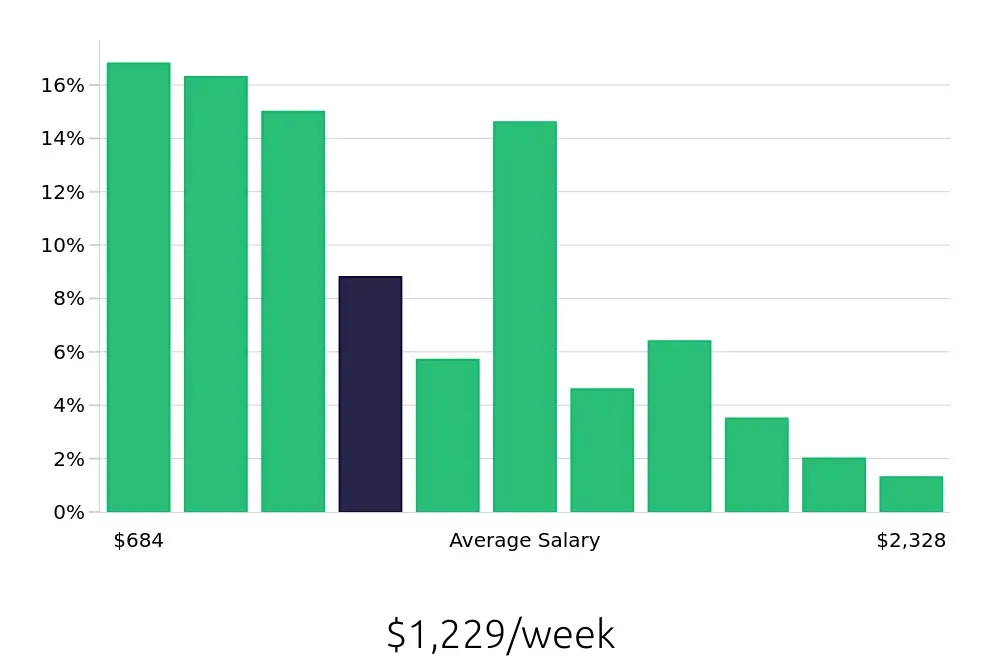
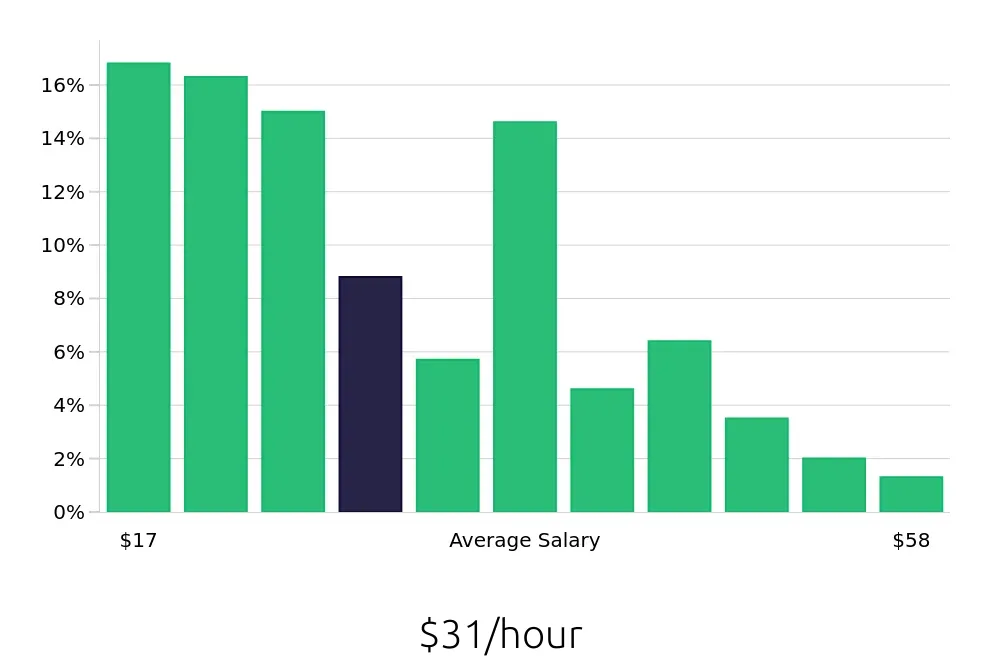
A Clinical Appeals Reviewer examines healthcare claims to ensure they are correct. These reviewers work to improve the fairness of healthcare decisions. Their salary can vary based on experience and location. The average yearly salary for a Clinical Appeals Reviewer is about $63,884. However, salaries can range widely. Some reviewers earn as little as $35,560 per year, while others make up to $121,072.
The salary of a Clinical Appeals Reviewer often increases with more experience. For instance, those with less than a year in the field might earn around $35,560. As experience grows, so can the salary. Reviewers with five to ten years of experience often earn between $74,429 and $89,977. Top earners, with more than ten years of experience, can reach up to $121,072 per year. This progression shows a clear path for growth in this career.
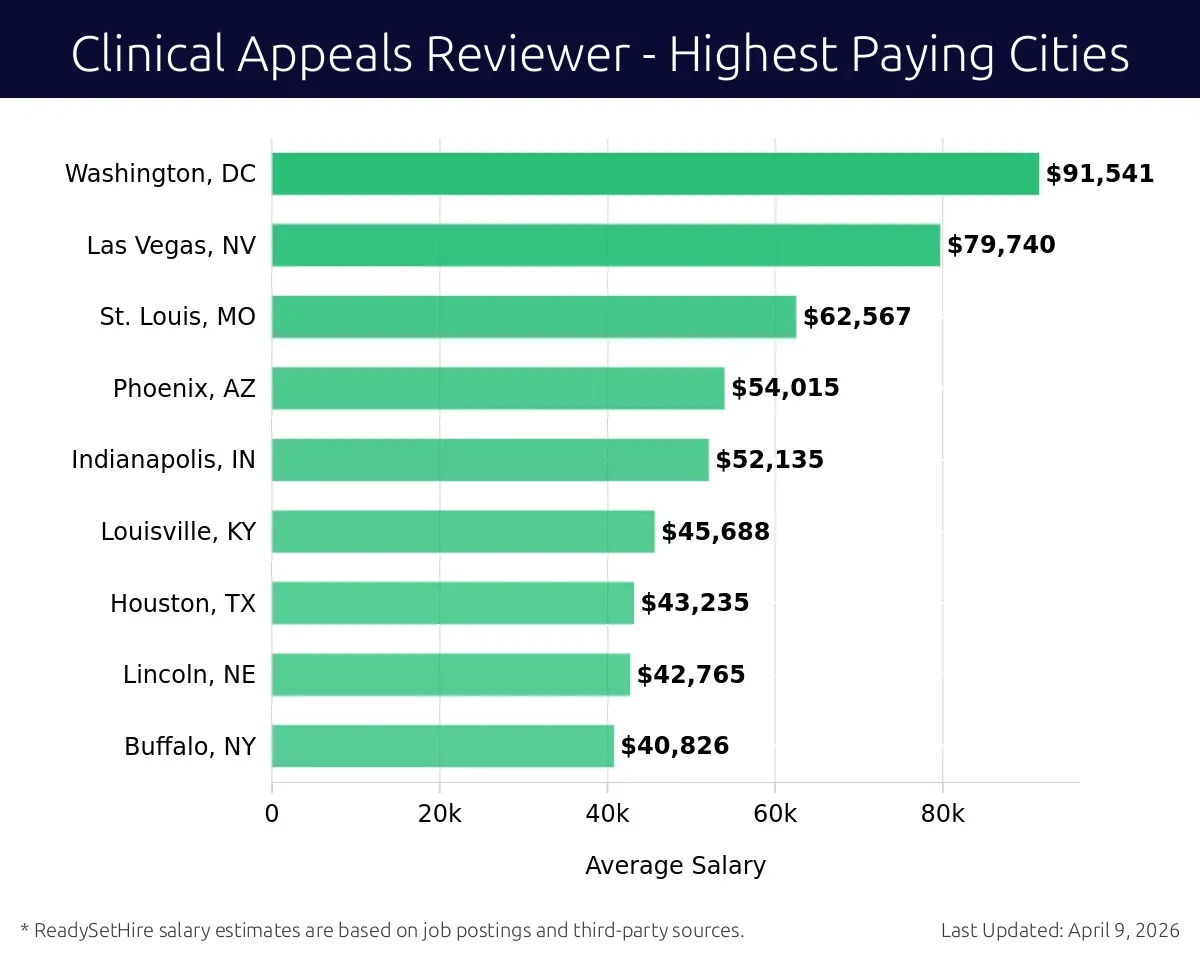
What are the highest paying cities for a Clinical Appeals Reviewer?
-
Washington, DC
Average Salary: $91,541
In Washington, DC, this role is crucial in ensuring fair treatment for patients. Many prominent healthcare organizations seek skilled reviewers who can navigate complex regulations. With a strong economy and many job opportunities, it's an excellent place for professionals to excel.
Find Clinical Appeals Reviewer jobs in Washington, DC
-
Las Vegas, NV
Average Salary: $79,740
Working as a reviewer in Las Vegas offers a vibrant environment with many healthcare facilities. Reviewers here focus on resolving disputes efficiently. The city's booming healthcare sector provides ample chances for career growth and development.
Find Clinical Appeals Reviewer jobs in Las Vegas, NV
-
St. Louis, MO
Average Salary: $62,567
In St. Louis, this position involves reviewing claims for fairness. It's a key role in maintaining the quality of healthcare services. The city offers a stable job market and a range of professional development opportunities.
Find Clinical Appeals Reviewer jobs in St. Louis, MO
-
Phoenix, AZ
Average Salary: $54,015
Phoenix provides a dynamic setting for reviewing medical claims. Professionals here work to ensure patients receive the care they deserve. The city’s healthcare industry is growing, offering various career advancement opportunities.
Find Clinical Appeals Reviewer jobs in Phoenix, AZ
-
Indianapolis, IN
Average Salary: $52,135
Indianapolis is an excellent place for reviewers to work. They play a vital role in healthcare, ensuring fairness. The city has many healthcare providers, making it a stable job market with good growth prospects.
Find Clinical Appeals Reviewer jobs in Indianapolis, IN
-
Louisville, KY
Average Salary: $45,688
In Louisville, this job means reviewing claims to ensure patient rights are protected. It’s an essential role in the city's healthcare system. The area's healthcare sector offers many opportunities for career development.
Find Clinical Appeals Reviewer jobs in Louisville, KY
-
Houston, TX
Average Salary: $43,235
Houston offers a thriving job market for healthcare reviewers. They work to resolve disputes and ensure patients receive proper care. The city's diverse healthcare industry provides many opportunities for growth.
Find Clinical Appeals Reviewer jobs in Houston, TX
-
Lincoln, NE
Average Salary: $42,765
Lincoln provides a supportive environment for healthcare reviewers. They focus on resolving claims to ensure fair treatment. The city's healthcare sector is growing, offering many opportunities for professional development.
Find Clinical Appeals Reviewer jobs in Lincoln, NE
-
Buffalo, NY
Average Salary: $40,826
Buffalo offers a stable job market for healthcare reviewers. They work to ensure patients receive the care they need. The city’s healthcare industry provides many opportunities for career advancement.
Find Clinical Appeals Reviewer jobs in Buffalo, NY
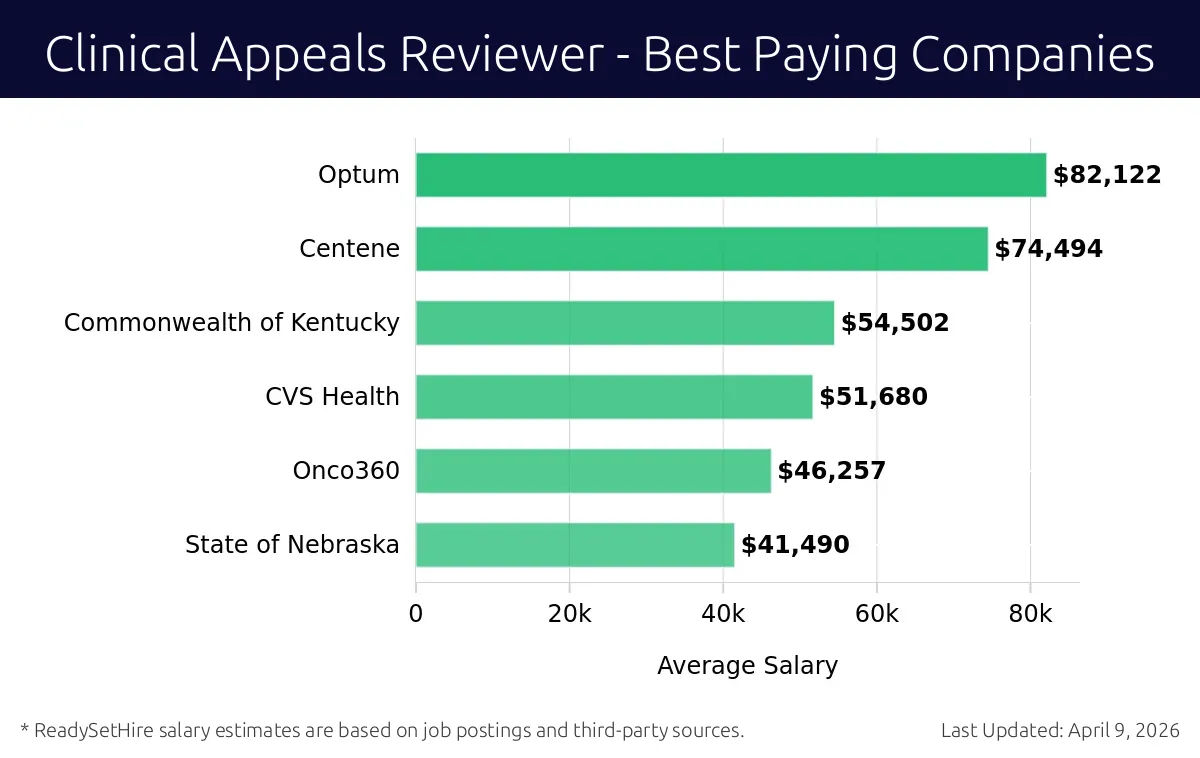
What are the best companies a Clinical Appeals Reviewer can work for?
-
Optum
Average Salary: $82,122
Optum offers Clinical Appeals Reviewer jobs with a strong focus on healthcare management. They have locations across the United States, providing diverse opportunities for professionals. Their reviews ensure fair patient care decisions. Employees enjoy competitive salaries and comprehensive benefits.
-
Centene
Average Salary: $74,494
At Centene, Clinical Appeals Reviewers work in ensuring patient claims are processed correctly. They serve communities nationwide. The role requires attention to detail and a good understanding of healthcare policies. Centene provides a supportive work environment and opportunities for career growth.
-
Commonwealth of Kentucky
Average Salary: $54,502
The Commonwealth of Kentucky offers Clinical Appeals Reviewer jobs with a focus on public service. They operate across Kentucky, providing essential healthcare services. This role involves reviewing medical claims to ensure accuracy. The position offers stability and a chance to serve the community.
-
CVS Health
Average Salary: $51,680
CVS Health provides Clinical Appeals Reviewer positions with a focus on pharmacy and healthcare services. They have locations throughout the United States. Reviewers ensure that patient claims are handled correctly. The role includes working with various healthcare providers and supporting patients’ needs.
-
Onco360
Average Salary: $46,257
Onco360 offers Clinical Appeals Reviewer jobs with a focus on cancer care support services. They operate in several states across the U.S. Reviewers ensure fair handling of patient claims related to cancer treatments. This role supports patients and healthcare providers in navigating complex claims.
-
State of Nebraska
Average Salary: $41,490
The State of Nebraska provides Clinical Appeals Reviewer positions that focus on public health. They operate within Nebraska. Reviewers ensure that medical claims are processed accurately. This role offers a chance to work in a public service environment and support community health initiatives.
How to earn more as a Clinical Appeals Reviewer?
Being a Clinical Appeals Reviewer offers a rewarding career path with the potential for earning more over time. This role involves reviewing healthcare appeals to ensure that patients receive the care they need. With the right approach, professionals can increase their earnings. The following factors can help achieve higher pay:
- Experience: More years of experience often lead to higher pay. As a reviewer gains expertise, they can handle more complex cases and take on leadership roles.
- Certification: Obtaining certifications in healthcare can boost earnings. Many employers value certifications like Certified Professional Coder (CPC) or Certified Healthcare Access Associate (CHAA).
- Education: Higher levels of education, such as a degree in healthcare administration or a related field, can lead to higher salaries. Continuous learning and professional development also play a role.
- Skill Set: Developing a strong skill set, including proficiency in medical coding, excellent communication skills, and a thorough understanding of healthcare policies, can increase earning potential.
- Performance: Top performers who consistently meet or exceed expectations often earn more. Demonstrating a high level of accuracy and efficiency can lead to bonuses and promotions.
Pursuing these factors can help Clinical Appeals Reviewers earn more and advance their careers. With dedication and continuous improvement, the earning potential grows significantly.