What does a Credentialing Specialist do?
A Credentialing Specialist plays a crucial role in ensuring that healthcare professionals meet all necessary qualifications. This role involves verifying the education, licenses, and certifications of medical staff. Specialists review documents to confirm that practitioners are qualified to work in their field. This task helps maintain high standards in healthcare settings.
Credentialing Specialists interact with various departments within a healthcare facility. They work closely with human resources, compliance, and medical staff offices. Specialists must have strong attention to detail and excellent organizational skills. They ensure all staff have up-to-date credentials, which is vital for patient safety and compliance with regulations. This position is essential for smooth operations in any healthcare environment.
How to become a Credentialing Specialist?
Becoming a Credentialing Specialist offers a rewarding career path in the healthcare industry. This role focuses on verifying the qualifications of healthcare professionals. It requires attention to detail and a solid understanding of regulatory requirements. A career in this field can lead to job satisfaction and opportunities for growth.
To embark on this career, follow a structured process that includes education, certification, and practical experience. The steps below provide a clear outline to guide professional job seekers toward becoming a Credentialing Specialist.
- Earn a High School Diploma or GED: The first step involves completing high school or obtaining a GED. This forms the foundation for further education and training.
- Gain Relevant Experience: Work in roles related to healthcare administration or medical records. This experience helps build the skills needed for credentialing.
- Complete a Training Program: Enroll in a certificate or associate degree program in health information management or a related field. Programs often cover topics like medical coding and healthcare regulations.
- Obtain Certification: Get certified through recognized organizations such as the National Association of Healthcare Access Management (NAHAM) or the American Academy of Professional Coders (AAPC). Certification can enhance job prospects and credibility.
- Apply for Jobs: Start applying for credentialing specialist positions. Use job boards, company websites, and networking to find opportunities. Tailor the resume to highlight relevant skills and experiences.
How long does it take to become a Credentialing Specialist?
Interested in a role that balances healthcare and administrative tasks? The journey to becoming a Credentialing Specialist often starts with gaining the right education and experience. Most enter the field with a high school diploma and pursue a certificate program in medical coding or healthcare administration. These programs typically last from a few months to a year, offering essential training in patient record management, insurance, and compliance.
After completing a certification program, gaining hands-on experience becomes key. Many specialists start in entry-level roles in healthcare settings. This experience allows for the development of skills in verifying credentials, ensuring compliance with regulations, and processing paperwork efficiently. Working in this capacity can take several months to a year, depending on the individual's dedication and the hiring needs of the organization.
Credentialing Specialist Job Description Sample
A Credentialing Specialist is responsible for managing the credentialing process for healthcare providers, ensuring compliance with regulatory standards, and facilitating the timely verification of provider qualifications.
Responsibilities:
- Verify and collect necessary documentation from healthcare providers to support credentialing applications.
- Review and assess provider credentials, licenses, certifications, and other relevant documents for accuracy and completeness.
- Maintain up-to-date records of provider credentials and ensure timely renewal and updates.
- Collaborate with healthcare providers to resolve any issues or deficiencies in their credentialing applications.
- Ensure compliance with state and federal regulations, as well as organizational policies, related to credentialing processes.
Qualifications
- Bachelor's degree in Healthcare Administration, Business Administration, or a related field.
- Minimum of 3-5 years of experience in healthcare credentialing, medical billing, or a related field.
- Strong knowledge of healthcare regulatory requirements, such as those set by the Joint Commission, NCQA, and state medical boards.
- Excellent organizational and time-management skills.
- Strong attention to detail and accuracy in document review and record-keeping.
Is becoming a Credentialing Specialist a good career path?
A Credentialing Specialist plays a crucial role in ensuring healthcare providers meet necessary qualifications. This role involves verifying licenses, certifications, and other important credentials. Credentialing Specialists must stay updated on laws and regulations to ensure compliance. Their work helps keep patient care safe and up to standards.
This career offers several benefits. Specialists enjoy the satisfaction of maintaining high standards in healthcare. They often work in a stable environment with predictable schedules. Networking opportunities with other healthcare professionals can also lead to career growth. However, some challenges exist. Specialists may face repetitive tasks and tight deadlines. The job can also involve handling sensitive information, requiring a high level of confidentiality.
Consider these pros and cons before pursuing this career:
- Pros:
- Stable job environment
- Predictable work schedule
- Opportunities for professional growth
- Contribution to patient safety and quality care
- Cons:
- Repetitive tasks
- Tight deadlines
- Handling sensitive information
What is the job outlook for a Credentialing Specialist?
The job outlook for Credentialing Specialists looks promising for job seekers. The Bureau of Labor Statistics (BLS) shows an average of 84,100 job positions per year from 2022 to 2032. This reflects a positive growth trend, suggesting many opportunities in the field. The BLS also projects a 5.4% increase in job openings from 2022 to 2032. This indicates a stable and growing demand for Credentialing Specialists.
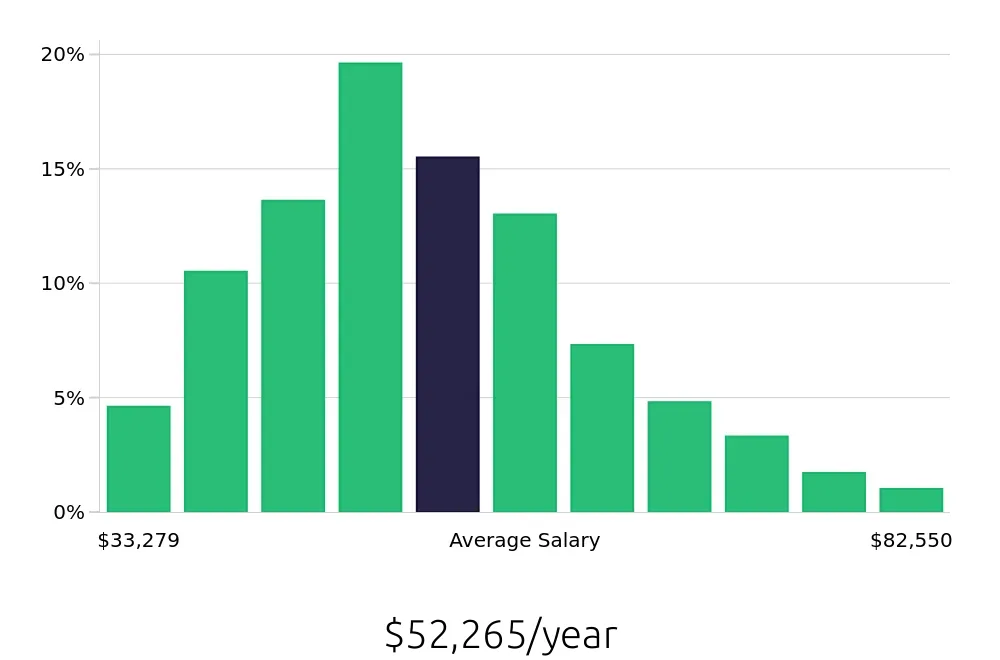
For those considering this career, the financial rewards are worth noting. The BLS reports an average national annual compensation of $77,260. This competitive salary reflects the value employers place on qualified Credentialing Specialists. Hourly compensation averages $37.15. This means that those in this role can expect a fair wage for their expertise and efforts. The high demand and good pay make this a great field to explore for job seekers.
Credentialing Specialists can look forward to a positive job outlook and good compensation. The growing number of job openings and rising demand highlight a strong need for skilled professionals. With a stable job market and a competitive salary, this career path offers stability and financial benefits. Job seekers interested in healthcare administration will find this field both rewarding and promising.
Currently 329 Credentialing Specialist job openings, nationwide.
Continue to Salaries for Credentialing Specialist